
WHAT IS OSTEOPOROSIS?
Osteoporosis, which literally means Porous Bone, is a disease in which the density and quality of bone are reduced. As bones become more porous and fragile, the risk of fracture is greatly increased. The loss of bone occurs silently and progressively. Often there are no symptoms until the first fracture occurs.
What causes osteoporosis?
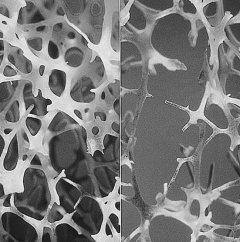
Left: Normal Bone, Right: Osteoporotic Bone.
Our bones are living tissue and constantly changing. From the moment of birth until young adulthood, bones are developing and strengthening. Our bones are at their most dense in our early 20's – called peak bone mass.
See more detailed information about Bone Biology.
WHO'S AT RISK?
Because bone loss is gradual and painless, there are usually no symptoms to indicate a person is developing osteoporosis. This is why osteoporosis is often referred to as the silent disease. Often the first symptom of osteoporosis is a fracture. Most commonly, osteopo rotic fractur es occur at the spine, the wrist or the hip, althou gh osteoporotic fractures can occur in other bones as well.
While most limb fractures (such as at the wrist or hip) are obvious, spinal fractures can be more difficult to diagnose. This is because they might be painless, or if there is pain, a person may not know it is caused by a fracture due to the many different causes of back pain.
More obvious signs of spinal fractures are:
- Loss of height
- Development of a curved upper back (sometimes called a Dowager's Hump)
Since there are usually no outward signs of osteoporosis developing, doctors will often recommend diagnostic testing depending on your age and if you have other risk factors for the disease1.
What are your osteoporosis risk factors?
A risk factor is anything that increases your chance of getting a disease. Having a risk factor, or even several, does not mean that you will have osteoporosis. However, the more risk factors you have, the greater your chance of developing a disease and also, the greater the level of each risk factor, the greater the risk2. There are different kinds of risk factors - fixed and modifiable.
Some factors, such as age or gender, cannot be changed; whereas, others are linked to personal lifestyle choices, such as smoking, alcohol intake and diet.
Fixed risks
Although fixed risk factors cannot be changed, people need to be aware of them so that they can take steps to reduce bone mineral loss. Fixed risk factors also include what is termed ‘secondary risk factors’ – disorders and medications that weaken bone and affect balance (heighting the risk of fracture due to falling)
Fixed riskfactors include 3-6:
- Age
- Female gender
- Family history of osteoporosis
- Previous fracture
- Ethnicity
- Menopause/hysterectomy
- Long term glucocorticoid therapy
- Rheumatoid arthritis
- Primary/secondary hypogonadism in men
PREVENTING OSTEOPOROSIS
Genetic factors play a significant role in determining whether an individual is at heightened risk of osteoporosis. However,lifestyle factors such as diet and physical activity also influence bone development in youth and the rate of bone loss later in life.
After your mid-20's, bone thinning is a natural process and cannot be completely stopped. The thicker your bones, the less likely they are to become thin enough to break. Young women in particular need to be aware of their osteoporosis risk and take steps to slow its progress and prevent fractures.
Childhood to adolescence

Invest in bone health.
The prevention of osteoporosis begins with optimal bone growth and development in youth. Bones are living tissue, and the skeleton grows continually from birth to the end of the teenage years, reaching a maximum strength and size (peak bone mass) in early adulthood, around the mid-20s. Read about bone development in young people.
Children and adolescents should:
- Ensure a nutritious diet with adequate calcium intake
- Avoid protein malnutrition and under-nutrition
- Maintain an adequate supply of vitamin D
- Participate in regular physical activity
- Avoid the effects of second-hand smoking
It’s estimated a 10% increase of peak bone mass in children reduces the risk of an osteoporotic fracture during adult life by 50%.
Adulthood
Bone mass acquired during youth is an important determinant of the risk of osteoporotic fracture during later life. The higher the peak bone mass, the lower the risk of osteoporosis. Once peak bone mass has been reached, it is maintained by a process called remodelling. This is a continuous process in which old bone is removed (resorption) and new bone is created (formation). The renewal of bone is responsible for bone strength throughout life.
During childhood and the beginning of adulthood, bone formation is more important than bone resorption. Later in life, however, the rate of bone resorption is greater than the rate of bone formation and results in net bone loss –a thinning of your bones.
Any factor which causes a higher rate of bone remodelling will ultimately lead to a more rapid loss of bone mass and more fragile bones. The nutritional and lifestyle advice for building strong bones in youth is just as applicable to adults to.
Adults should:
- Ensure a nutritious diet and adequate calcium intake
- Avoid under-nutrition, particularly the effects of severe weight-loss diets and eating disorders
- Maintain an adequate supply of vitamin D
- Participate in regular weight-bearing activity
- Avoid smoking and second-hand smoking
- Avoid heavy drinking
DIAGNOSING OSTEOPOROSIS
Men and women over 60-years-old are at higher risk of osteoporosis than younger people. Nevertheless, it is possible to have osteopenia (low bone mass) or osteoporosis at a much earlier age. As osteoporosis has no obvious symptoms, it's important to go to your doctor if any risk factors apply to you.
By making positive lifestyle changes and following appropriate treatment strategies in consultation with a doctor, osteoporotic fractures can be prevented. Your doctor will take a thorough medical history that includes information on any recent fractures and may determine the next step is to have a bone mineral density (BMD) test.
What is a BMD test?
Traditional X-rays can’t measure bone density, but they can identify spine fractures. Bone mineral density (BMD) has to be measured by more specialised techniques. A number of different types of BMD tests are available, but the most commonly used is DXA (dual-energy X-ray absorptiometry) DXA is a low radiation X-ray capable of detecting quite small percentages of bone loss. It is used to measure spine and hip bone density, and can also measure bone density of the whole skeleton. There are a number of different types of test options [1]:
• DXA (peripheral DXA) measures bone mass.
A DXA scan, which is used to measure spine and hip bone density, is the most common technique for assessing the risk of osteoporosis.
What do my test results mean?
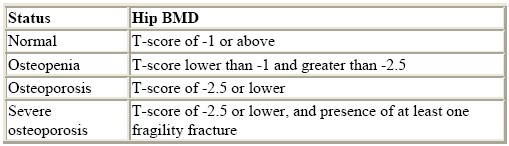
The World Health Organization has defined a number of threshold values (measurements) for osteoporosis. The reference measurement is derived from bone density measurements in a population of healthy young adults (called a T-score).
Osteoporosis is diagnosed when a person’s BMD is equal to or more than 2.5 standard deviations below this reference measurement [2].
Osteopenia is diagnosed when the measurement is between 1 and 2.5 standard deviations below the young adult reference measurement.

If the results of your BMD test show osteopenia or osteoporosis, it does not automatically mean that you will have a fracture. There are lifestyle changes and a number of available therapies that your doctor might prescribe to slow down bone loss and help prevent fractures.
Hologic Takes Action to Advance Skeletal Health Imaging
Our bones and joints give us stability and mobility, the freedom to move and the strength to perform. Young and old, men and women - everyone shares the same dependence on a strong, healthy skeletal structure. It is something e all take for granted.
For many years Hologic has set the gold standard in osteoporosis assessment. Now we are expanding our solutions to address the continuum of skeletal health care, from prevention to intervention. Just as we are leading the way in women's health imaging solutions, we are raising the bar in skeletal health imaging. We want to give our customers the very best tools to address one of the world's most devastating health problems. Our goal is to be the strong foundation that clinicians rely on in their fight for better skeletal health for everyone.

Osteoporosis Assessment and Beyond
Osteoporosis is a growing healthcare crisis affecting millions of women and men worldwide. The healthcare costs associated with osteoporosis are staggering, and the effect on your patient's quality of life can be devastating.
Fortunately, osteoporosis is detectable and treatable. Our bone densitometry systems offer you a single platform to support a broad spectrum of patients.
They not only provide you with superb diagnostic tools to support the early detection and treatment of osteoporosis, but offer a very comprehensive platform for bone health assessment, obesity assessment, visualization of calcification in the abdominal aorta that can indicate heart disease1, and many other clinical applications.
Designed for Efficient Workflow
The Discovery dual energy X-ray absorptiometry (DXA) system provides a single comprehensive platform for the assessment of three major health issues: osteoporosis including vertebral fracture assessment, cardiovascular disease, and obesity.
Discovery delivers:
• Exceptional Precision and Accuracy
• High Definition Digital DXA Detectors - To improve fracture detection and to visualize abdominal aortic calcifications1.
• Speed and Image Quality - Discovery imaging technology captures the hip and spine with as fast as 10-second regional scanning time.
• Superb Visualization1 - The Discovery system's exclusive design utilizes a high resolution detector array paired with true fan-beam linearacquisition geometry.
• Consistency from Exam to Exam - The Discovery system performs continuous, automatic calibration, ensuring precise measurements results from exam to exam.
Superior Fracture Risk Assessment
Hologic pioneered the next generation of vertebral fracture assessment (VFA) technology, High Definition Instant Vertebral Assessment (IVA-HD), which dramatically improves the detection of vertebral fractures. IVA-HD doubles the resolution of previously available techniques with a low-dose, single-energy image, integrating important definitive factors for osteoporotic fracture risk: BMD and VFA.
Advanced Body Composition Assessment with InnerCore Visceral Fat Assessment For more than three decades, the prevalence of obesity has increased rapidly among both adults and children. In 2008, 1.5 billion adults, 20 and older, were overweight. Of these, over 200 million men and nearly 300 million women were obese1. The demand for accurate body composition analysis is growing as healthcare providers realize its value in identifying serious health risks that result from obesity, including heart disease and type 2 diabetes2. The Advanced Body Composition assessment feature produces color images displaying the distribution of fat, lean mass, bone, and fat mass index translating the information into an easy to interpret report for improved patient management and counselling.
Hologic whole body DXA systems are the only ones to incorporate the National Health and Nutrition Examination Survey (NHANES) whole body composition reference data. Combined with the recently released guidelines from the Endocrine Society which recommends annual bone mineral density and body composition exams for bariatric surgery patients3, the Discovery DXA system will enable you to improve patient management by not only offering bone mineral density tests, but by also calculating your patient's body composition.
FRAX®* 10-year Fracture Risk Assessment
Identify patients who otherwise would go untreated Now you can identify and proactively treat patients with a high risk of fracture due to low bone density and other risk factors. We are excited to be the first to make the FRAX 10-year fracture risk calculator commercially available through our Discovery osteoporosis risk evaluation tools.
The FRAX calculator will help you to identify patients who are at high risk of experiencing fractures within a period of 10 years, by combining eleven of the highest risk factors, including age, personal history of fractures, and family history of fractures, plus country-specific life expectancy and country-specific fracture data. The FRAX calculator identifies patients who are at high risk of fracture but would not be candidates for preventative therapy using the traditional T-score of -2.5.
By incorporating the FRAX calculator into our Discovery bone densitometer systems, we will help dramatically alter and improve the way patients are evaluated and treated for potential bone fractures and will maintain our ongoing commitment to provide the most up-to-date technology combating osteoporosis.
We continue to provide exceptional tools to identify patients at risk for costly fractures. Our mission is to greatly reduce the medical, emotional and economic burden that osteoporosis places on this country, and the world.